Whose Birthing Practices?
In the United States, women and women's networks oversaw and managed birthing practices with little intervention until the mid-1800s. As a fledgling medical establishment sought greater control in the late 19th century, tensions arose between "irregular" and "regular" health professionals who practiced in pregnancy and birth. The former often included midwives trained in traditional healing practices associated with their cultural or ethnic provenance. The latter consisted of formally educated – and eventually state-licensed – physicians, nurses, and nurse-midwives.
Birth advocates in the reproductive justice movement today recognize that women of color and poor women not only have fewer choices in birth, but experience disparate outcomes. The images in “Whose Birthing Practices” illustrate who attends the birth, where it takes place, and whose agency is privileged in the process. As with reproductive bodies, birthing practices have been and are significantly stratified depending on race, ethnicity, socio-economic status, gender identity, sexuality, and disability.
Birth Moves to the Hospital
In 1933, 35% of all births occurred in hospitals; by 1955 this had risen to 95%. Hospitals became increasingly attractive sites for birth with medical innovations such as twilight sleep, which combined morphine and scopolamine to sedate women during delivery. Hospital birth often diminished women’s agency by an insistence on a woman's supine position throughout labor and birth, restraint of hands and feet, and with a ban on all family and friends from the delivery room. Even within this historical context, many obstetricians, such as Dr. Reuben Peterson, a University of Michigan physician who ran a busy private hospital and nurse’s training school in Ann Arbor in the early 20th century, offered middle-class women high quality care.
Nurse-Midwives Reach Out
With the elimination of traditional midwives, many poor urban and rural women lost access to care. A new kind of practitioner, the nurse-midwife, emerged. The Frontier Nursing Service, established by Mary Breckinridge in 1925, deployed nurses on horseback to serve Kentucky families. In the early 20th century, as states put licensure requirements in place, nurses and nurse-midwives began to oversee and in many instances replace traditional midwives.
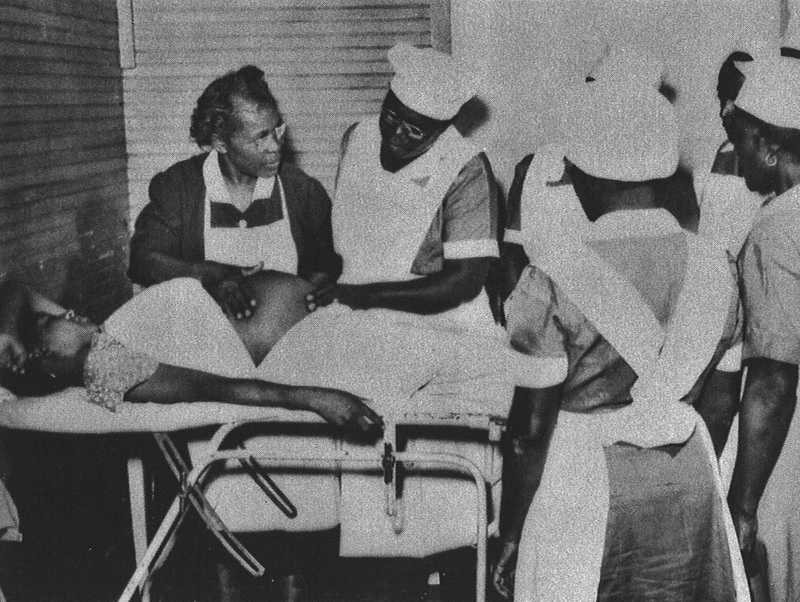
Grand Midwives Versus the AMA
African-American communities in the South enjoyed a strong tradition of Grand (or "Granny") Midwives. The lineage of these respected midwives originated in Africa and survived the times of slavery. They were often the sole health care providers for their communities. In the mid-19th century, “regular” physicians, riding the wave of medical professionalization, began to challenge rival practitioners. In Chicago, home of the newly-founded American Medical Association, physicians advocated solving "The Midwife Problem" with legal measures designed to dismantle midwifery practice, disproportionately impacting African-American and foreign-born midwives.
Our Bodies, Our Births
In the 1960s and 70s, women began to demand greater rights in childbirth. Some hospitals increased amenities in labor and delivery rooms, admitting husbands, and introducing nurse-midwife services. A movement to reinvent traditional midwifery started with Ina May Gaskin, the founder of The Farm midwifery center in Tennessee. Despite proven effectiveness, these new midwives faced opposition from medical leadership as well as government bodies.
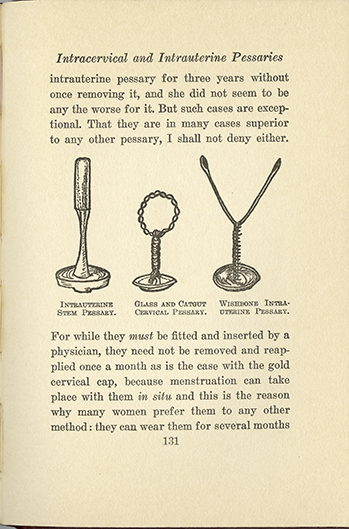
Whose Knowledge?

Reproductive Justice Today